By Meru Sheel and Allen Cheng
Typically, an uptick in influenza cases is expected as winter approaches, but this year has proven to be different, with approximately 25,000 cases reported between January and March. This figure represents only a small portion of the actual cases.
While most individuals recover from the flu without medical intervention, it poses significant health risks for vulnerable groups, including the elderly, young children, pregnant women, and those with chronic health conditions such as asthma or heart disease. Annually, influenza is responsible for around 3,500 deaths in Australia and results in approximately 18,000 hospitalizations.
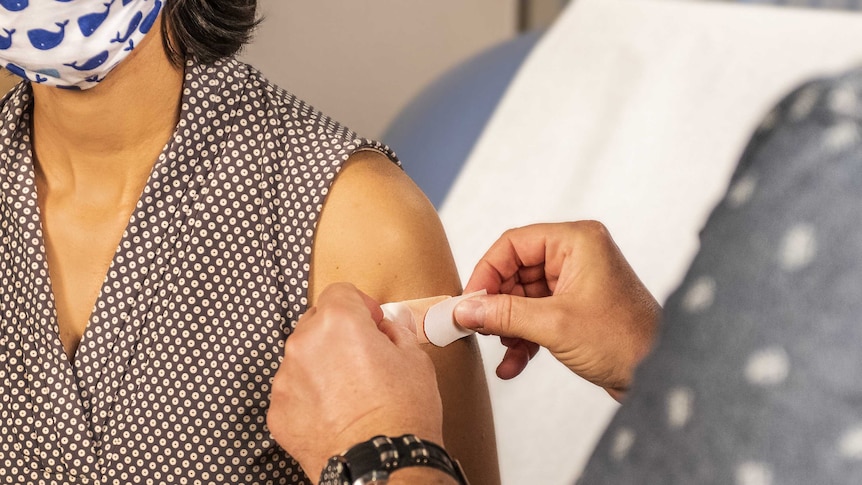
The most effective means of protection against the flu is vaccination, which is recommended for everyone aged six months and older. Certain high-risk groups are eligible to receive the vaccine at no charge. Others can obtain it, typically for a fee, at pharmacies, general practitioner clinics, and local council clinics across various states and territories. Additionally, some employers provide vaccinations for their employees.
Since the onset of the COVID-19 pandemic, influenza patterns have become less predictable, with instances of flu occurring outside the typical season. Furthermore, research indicates that immunity may decline towards the end of winter. This raises the question: when is the optimal time to get vaccinated?
Flu symptoms generally manifest as a cough, sore throat, fever, body aches, and fatigue. The virus spreads through respiratory droplets produced when an infected person talks, coughs, or sneezes. It can also be transmitted by touching contaminated surfaces, although this method is less common. If you are experiencing flu symptoms, it is advisable to remain at home.
Influenza transmission tends to increase during winter months, largely due to people spending more time indoors and in close proximity to one another. Some studies suggest that the virus spreads more effectively in colder temperatures.
This year’s flu is primarily associated with four strains: A(H3N2), A(H1N1), B/Victoria, and B/Yamagata. In Australia, nearly 98% of reported cases are linked to the A(H3N2) strain, with the remainder attributed to B/Victoria. A new variant of the H3N2 strain, referred to as “super-K,” emerged during the Northern Hemisphere winter and has been linked to the increased flu cases seen over the summer in Australia. However, there is currently no evidence suggesting it is more severe than other H3N2 variants.
The flu vaccine for this year has been formulated to combat a variety of circulating virus strains. It includes components targeting the A(H1N1)pdm09 and A(H3N2) subtypes, as well as a B strain. Specifically, it comprises an A/Missouri/11/2025 (H1N1)pdm09-like virus, an A/Singapore/GP20238/2024 (H3N2)-like virus, and a B/Austria/1359417/2021 (B/Victoria lineage)-like virus. Notably, the Singapore strain in this year’s vaccine is closely related to the super-K variant, potentially offering improved protection compared to last year’s vaccines in both hemispheres.
At this stage, it is premature to assess the effectiveness of this year’s vaccine in preventing infection and severe illness. Preliminary data suggests that individuals vaccinated in 2025 were 53% less likely to require hospitalization or seek medical attention for flu symptoms compared to those who were unvaccinated. During the Northern Hemisphere winter of 2025-26, flu vaccines in the UK demonstrated an effectiveness rate of 72-75% in preventing medically attended flu cases among children and adolescents, including those caused by the super-K strain. Vaccination can also help curb the transmission of the virus to others who cannot receive the vaccine.
From data collected in the United States prior to 2020, it was found that influenza vaccines were 21% effective in preventing infection among household members. Research conducted in the UK and Ireland between 2010 and 2017 indicated that vaccinating school-aged children significantly reduced the incidence of respiratory illnesses reported to general practitioners across all age groups.
The flu season in temperate Australia generally spans from May to October, peaking around June and July. Although flu cases can occur year-round, the ideal time to receive the flu vaccine is approximately two weeks before the onset of flu activity. However, this can be challenging to predict, as the increase in cases may begin anywhere from April to July in temperate regions, and even earlier in tropical areas of northern Australia.
Research indicates that the immunity provided by flu vaccines diminishes over a six-month period. The best immunity is typically reached around two weeks after vaccination. However, some studies suggest that the methodology used to measure vaccine effectiveness might not fully account for other influencing factors. Waning immunity may be more pronounced in specific populations and can also vary based on the mutations that occur in circulating flu strains throughout the season.
When determining the best time to get vaccinated, individuals may weigh the potential benefits of waiting against the risk of contracting the flu beforehand. It is generally recommended to obtain the vaccine when it becomes available and convenient, ideally around April or May. For individuals traveling to the Northern Hemisphere during the winter months, it is advisable to get vaccinated two to four weeks prior to departure. Pregnant women should consider receiving the influenza vaccine alongside RSV (respiratory syncytial virus) and pertussis vaccines starting from 28 weeks of gestation to ensure protection for both the mother and baby. Additionally, young children receiving their first flu vaccine should receive two doses spaced four weeks apart, allowing ample time for the second dose before the flu season begins.
Meru Sheel is a professor of infectious diseases and global health at the University of Sydney. Allen Cheng is a professor of infectious diseases at Monash University. This article was first published on…